
Our vision is to create a new model of care, joining up primary and community mental health that:
- responds to local people’s needs quickly and easily
- removes thresholds and barriers to access.
- helps people to live as well as possible in their communities.
Trauma – informed approach – what is it?
We have an ambition that Leeds will be ‘compassionate and mentally healthy city for everyone’. Part of this ambition means recognising the effects that psychological trauma can have on people. Leeds has developed a ‘trauma – informed charter’ to describe this.
A trauma – informed approach means our teams aim to understand more about people’s individual care needs. It is less about asking “what is wrong with you?” and more about asking “what happened to you, what have been your personal experiences?”. It places more emphasis on understanding a person’s difficulties within the context of their life, and of the community within which they live.
By using our knowledge of trauma, we can improve how well we do our jobs and deliver our service. A trauma – informed approach allows our care teams to build more trust with service users, promoting more therapeutic relationships which support healing and recovery. Also, it involves providing a safer environment which feels calm and comfortable. It recognises the often life – long impact of traumatic experiences; and seeks to offer a compassionate, non – judgemental response to distress – while also recognising people’s strengths and supporting them to move past their difficulties.
Similarly, the system also needs to provide a psychologically safe and protective environment for to the staff who work in it.
Building the vision
In 2021 the Leeds Community Mental Health Transformation programme undertook the Institute of Health Improvement’s 90 Day Learning Cycle. This is an approach of exploring complex challenges which may not have a clear starting point or proposition. It provides a phased approach to change, of trying things. Learning, adapting and then piloting new ways of working.
The result of this work was a hub model, providing integrated health and care series and designed to meet the following principles of care.
People with mental health problems will be enabled to:
- Access mental health care where and when they need it and be able to move through the system easily so that people who need intensive input receive it in the appropriate place, rather than face being discharged to no support.
- Manage their condition or move towards individualised recovery on their own terms, surrounded by their families, carers and social networks and supported in their local community.
- Contribute to and be participants in the communities that sustain them to whatever extent is comfortable to them.
Three test sites were chosen to pilot this new hub model, each aligned to, and managed by a local care partnership (LCP) made up of health, social care and third sector organisations. The pilot sites are:
- West Leeds, served by the West Leeds Primary Care Network (PCN)
- The Hatch (Burmantofts, Harehills and Richmond Hill Primary PCN and the Chapeltown PCN)
- Leeds Student Medical Practice (LSMP) and The Light PCN
How might these integrated hubs work?
The integrated hub is a way to describe a team of different organisations working together. They usually won’t be all together in one physical place for people to ‘drop in’.
We recognise the wealth of resources available within local communities that help people to look after their own mental health. Some people do already and will continue to get support, advice and guidance from within their community and never come to the Integrated Hub.
Of those that come to the Hub, a significant number of people will need a brief intervention, often involving only one or two practitioners, for a limited amount of time.
Others with more complex needs may need longer term support and are more likely to require multi-agency coordinated care to support a variety of different needs.
People can and will move through different parts of the system, but this does not mean they move out of the service or stop receiving support, it may just be in a different place or a different way.
Broadly, support offered to people referred to the integrated hubs in Leeds includes:
- Recognition and assessment of mental health problems leading to a shared understanding (formulation)
- Provisions of treatment, including social, psychological and pharmacological approaches
- Recognition and support and management of physical health problems
- Work with and support families, carers and loved ones
- Recognition of and enabling things that support good mental health using community resources, such as stable housing, having enough money, obtaining and maintaining employment or education.
The aim of the hubs is to integrate services so that people don’t fall through the gaps, but that services and types of support are blended together.
People can move through different parts of the system without unnecessary hurdles or can receive support somewhere in the middle. For example, this may be receiving multi – agency co – ordinated care while also accessing community resources.
The diagram below shows how services and systems will support people using the hubs.
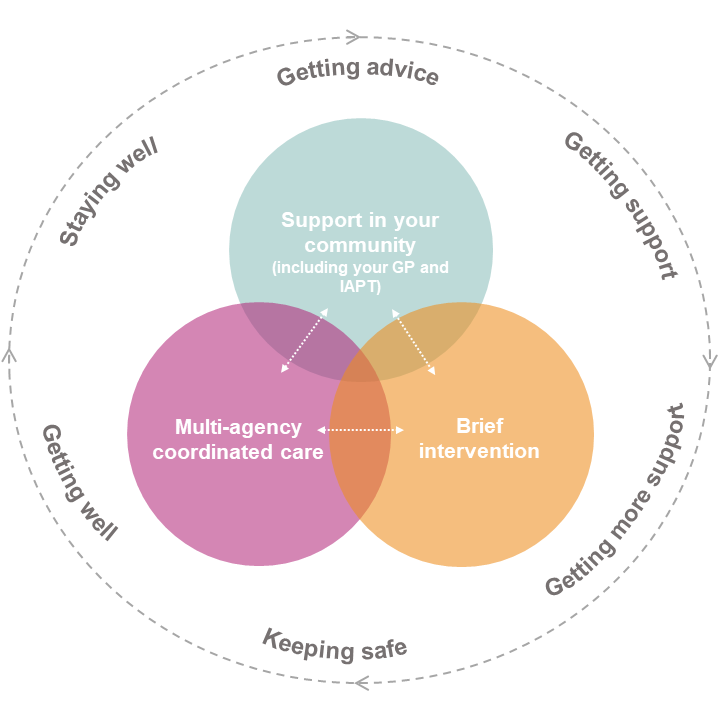
Referrals
- you can be referred to your local ‘hub’ by anyone, including your GP, self-referral, someone who loves and cares about you, anybody working in any community service in Leeds
- referrals will be simple, fast and flexible
- all referrals can be made by phone or online
- we will work with you to understand your needs and how they can best be met
- we will respond quickly to a referral (ideally within a day or two)
- we will share information about you sensitively and discreetly
Care and support available
Each hub will have a partnership of people and organisations providing personalised care and support designed for, and with you:
- providing mental and physical care and support
- providing a range of psychological therapies
- providing social care
- third sector agencies providing community support
- supporting you in your community e.g., housing, benefits, employment etc.
- sharing information only with people directly involved in your care
- providing care and support in places and ways that work best for you.
- providing support by a keyworker who you know, trust and can work with.
Hub staff
Although they may not be working in one place, each ‘hub’ of services and support will include (in alphabetical order):
- administrative staff
- clinical psychologists
- community wellbeing connectors / social prescribing link workers
- mental health nurses
- mental health pharmacists
- mental health practitioners (experienced but not ‘professionally’ registered)
- occupational therapists
- paid peer support workers / experts by experience
- primary care staff
- psychiatrists
- psychological therapists / psychotherapists
- social workers
- support workers – mental health, housing, employment, debt
- team managers / leaders
Life after the hub
We know it is important that while there is life after the hub, it will continue to be important. We will help you to move on when the time is right but always knowing you can call on help when you need it.
- your personalised care plan includes supporting you in your community after the hub, including:
- what keeps you well
- who is the right person to go to if things don’t go well
- preparing and agreeing a wellbeing plan / safety plan
- you can contact Leeds Crisis Services in an emergency if you need to after you leave the hub
- you can contact the hub any time after you are discharged (you will have contact details)
- we will respond to your needs whether you get better or worse.
The pilot sites will provide us with information about what works well, any changes that need to be made, and through feedback from users of services as well as our staff, what may be missing.
We will review this feedback to get things right at the first three sites, and in planning the second wave of hubs towards the end of 2023.
